
Finger Injuries in Young Climbers
While A and A4 pulley strains can occur in high-level youth athletes, growth plate injuries are much more common.
Learn more about how these injuries present themselves, to help you notice the issue early and take care of your fingers.
Growth Plate Injuries in Young Climbers
While A2 and A4 pulley strains can occur in high level youth athletes, (see Brian Squire’s review), growth plate injuries are much more common.
In adults the soft tissues, (pulleys and ligaments), are weaker than the bones, but in the adolescent climber who is actively growing, the growth plates at the end of the bones are the weakest link in the “chain”. Finger bones are considered long bones and grow by a process of endochondral ossification, where the end lengthens. This diagram below depicts the growth plates in blue, including when they appear on x-rays and when they fuse, (the bone becomes one solid piece).
Adolescents who get passionate about climbing often develop pain in the middle finger (MF) > ring finger (RF) at the proximal interphalangeal joint (PIPJ) without any particular inciting incident. It seems to come on with increased hours of training and is asymptomatic when at rest. The pain is often more acute and tenderness to touch is noted at the back (dorsal side) of the finger, not the palm side, (which is more common with a pulley injury). These joints will appear swollen compared to the other knuckles, as shown in the middle and ring fingers in the image below.
The crimp grip is the most uncomfortable one for them to use. Sometimes the pain in the finger precludes them from crimping on small holds.


Radiographs (X-rays) will often show widening of the growth plates (physes) on the dorsal aspect. This is a stress fracture due to overload, too much climbing and not enough rest or cross training. Sometimes these team athletes are training 4-5 days a week under the direction of their coaches but unbeknownst to their coaches, they are also projecting climbs or boulders on the weekends. Eventually their bodies will demand a break, particularly when they are actively growing, and their growth plates are relatively weak.

The good news? Over 99% of these injuries will heal up with rest, i.e. no climbing for a month, and then gradually building back a training base before returning to projecting climbs or boulders. During the time away from climbing, climbing team athletes are encouraged to train with their teammates in all other aspects of fitness including calisthenics, core, aerobic fitness but avoid any hang board, campus board, tension board, system board or Moon board training. It is an ideal time to increase chest and triceps strength and improve one’s max push-ups and sit-ups in 2 minutes for example. Work on flexibility and pistol squats which will pay dividends when climbing is allowed.
The not so good news? Sometimes it takes more than a month off to get better and allow the growth plates to heal. This is most often the case when the young climber has been training through pain and not sharing their discomfort with parents or coaching staff. In these cases, the growth plate can be more damaged and take several months to become pain-free.
These are radiographs of a 13-year-old girl who was winning competitions and climbing 5.13’s but dealing with MF pain for 2 years until it became too painful to climb. The physis is disrupted and fractured even as it is trying to close.



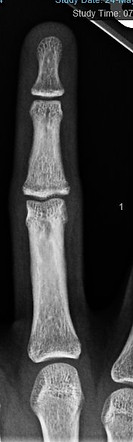
Luckily, she did heal up without any surgical intervention, but it took immobilization in a splint for 3 weeks and another 3 weeks off climbing until she successfully returned to climbing and eventually competitions. Here you can see improvement in the appearance of her physes with normal fusion occurring.
Pro tip: It is never wrong to see a hand surgeon with knowledge of treating climbers, to help make the diagnosis and treatment plan. Radiographic examinations are often helpful too.
Reference:
Bärtschi N, et al. Symptomatic Epiphyseal Sprains and Stress Fractures of the Finger Phalanges in Adolescent Sport Climbers. Hand Surg Rehab (2019).